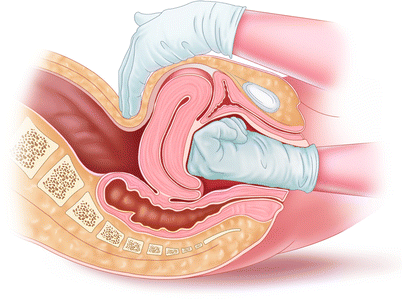
Uterine atony or atony of the uterus is a serious condition that can happen after childbirth. Uterine atony is a life-threatening condition and can result in maternal death. Immediate treatment is required if a woman goes experiences this condition.
In This Article:
- What Is Atony Of The Uterus?
- Symptoms Of Uterine Atony
- Causes Of Uterine Atony
- Risk factors Of Uterine Atony
- Diagnosis of Uterine Atony
- Complications Of Uterine Atony
- Treatment Of Uterine Atony
- Prevention Of Uterine Atony
What Is Atony Of The Uterus?
Uterine atony means the loss of tone in the uterine musculature. During labor, the uterine muscles contract, compressing the blood vessels and reducing the blood flow. This, in turn, increases the likelihood of coagulation and prevents hemorrhage. But when the uterus fails to contract after the delivery, it is known as atony of the uterus and this can lead to postpartum hemorrhage. It has been proved that 75%-80% of postpartum hemorrhages are due to uterine atony.
Symptoms Of Uterine Atony
The most common and foremost symptom of uterine atony is that the uterus remains relaxed and without any tension after giving birth. Atony of the uterus is the primary cause of postpartum hemorrhage. Postpartum hemorrhage is excessive bleeding post-delivery and occurs after the placenta is delivered. About 1%-5% of women have postpartum hemorrhage, and a loss of more than 500 millilitres of blood after delivery of the placenta is defined as postpartum hemorrhage. With most hemorrhages occurring right after delivery (especially in cesarean births), the symptoms include –
- Uncontrollable and excessive bleeding post-delivery of a baby
- A drop in blood pressure
- An increase in the heart rate
- Pain
- Back pain
Causes Of Uterine Atony
There are many factors that prevent the muscles of the uterus from contracting after labor. Some of the most common causes of uterine atony are –
- Prolonged laboror delayed labor
- Rapid labor
- Overdistention of the uterus (enlargement of the uterus) because of the presence of excess amniotic fluid (a condition called as polyhydramnios) or a large baby
- Administration of oxytocin, general anesthesiaor other drugs during labor
- Inducing laborusing medication
Risk factors Of Uterine Atony
There is a potential for an increased risk of the atony of the uterus if these factors exist –
- Multiple pregnancies or delivering twins or triplets
- Have had many previous deliveries
- Fetal macrosomia where the baby is larger than average
- If delivery was assisted using forceps or vacuum
- Age over 35 years
- Medically classified as obese
Diagnosis of Uterine Atony
Uterine atony is diagnosed when the uterus is soft, relaxed and there is an excess bleeding post giving birth to a baby. A doctor may be able to estimate the loss of blood by counting the number of saturated pads or weighing the sponges that are used to absorb blood. A physical examination by the doctor will help rule out other causes of bleeding like a tear in the cervix or pieces of the placenta in the uterus. The doctor will also keep a watch for the following –
- Pulse rate
- Blood pressure
- Count of red blood cells
- Factors for clotting of blood
Complications Of Uterine Atony
Apart from insufficient uterine contraction, other complications of uterine atony include –
- Giddiness, dizziness or light-headedness, due to low blood pressure generally termed as orthostatic hypotension
- Anemia
- Fatigue and tiredness
Anemia or fatigue after birth increases the chances of a mother experiencing postpartum depression. An uncontrolled and excessive loss of blood than the normal could lead to hemorrhagic shock. If blood loss is not monitored, then it could lead to a life-threatening situation.
Treatment Of Uterine Atony
The first treatment is intended to stop the bleeding and replace the blood that has been lost. Medical experts ensure that the mother is given iv fluids, blood, and blood products without any delay.
Other modes of treatment include –
- A uterine massage where the doctor places one hand in the vagina pushing against the uterus with the other hand over the abdominal wall compressing the uterus
- Prescribed uterotonic drugs including oxytocin, methylergonovine, and prostaglandins
- Blood transfusions
In the case where the conditions are severe, treatment includes –
- A surgery to tie the blood vessels
- Uterine artery embolization – it involves injecting minute and small particles into the uterine artery to impede blood flow to the uterus
- Hysterectomy, if all other treatments fail
Prevention Of Uterine Atony
Uterine atony cannot be prevented, but a doctor can help manage the condition through all the stages of labor. If there is a presence of risk, then appropriate uterine atony nursing management procedures must be in place. The medical facility should have iv lines ready, prescribed medications handy, and the equipment to deal with blood loss.
Vital signs of the amount of bleeding that occurred after birth must be monitored by the doctor to detect hemorrhage. Oxytocin is the first line of treatment suggested to help the uterus contract after delivery. Uterine massage has now become a common practice post-delivery of the placenta to reduce the risk of symptoms of uterine atony. Taking a regulated dose of prenatal vitamins and iron supplements can also help in preventing anemia and other complications of postpartum uterine atony.
Conclusion
Uterine atony is the main cause of primary postpartum hemorrhage, a condition marked by excessive bleeding. Scheduled and constant monitoring of the patient, access to a well-equipped hospital, availability of blood, blood products, drugs and the presence of competent medical staff at the time of delivery are vital for the diagnosis and prognosis of uterine atony.
References-